IMAGING
ULTRASOUNDS, THERMOGRAMS
ULTRASOUNDS
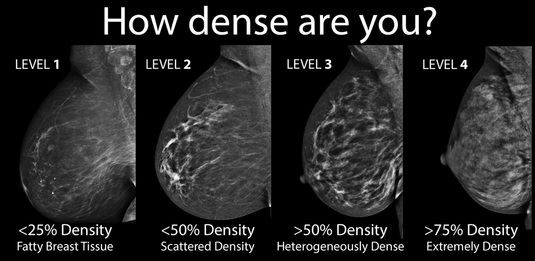
HAVE DENSE BREASTS? HARDER TO VISUALIZE PROBLEMS ON A MAMMOGRAM
MANY STATES REQUIRE NOTIFICATION OF FINDINGS OF BREAST DENSITY ON MAMMOGRAMS, AND THE NEED TO HAVE AN
ULTRASOUND.
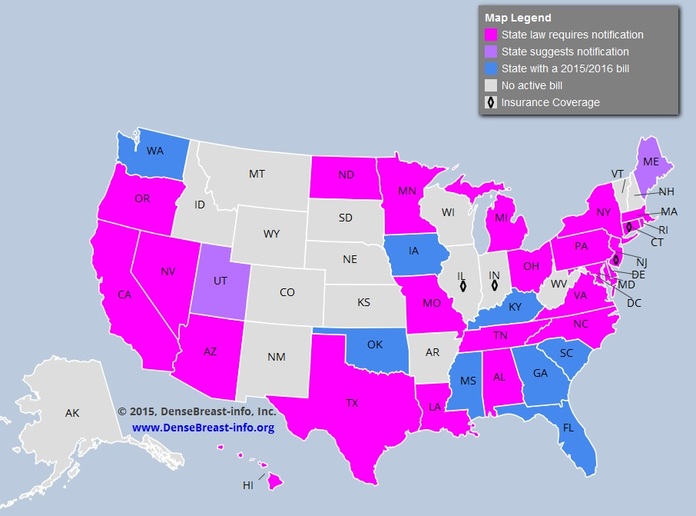
CHECK OUT YOUR STATE BELOW!
"Breast density is like mammogram's dirty little secret. Half of women over 40 have no idea that their 'normal' mammogram might not be normal at all. We are looking for a snowball in a snowstorm! You see, cancer is white, and dense tissue is white. So, dense breast tissue can overlap with cancers, masking them from view; in fact, we miss up to 50 percent of cancers in dense breasts. Secondly, dense tissue is the part of the breast that gets cancer, not fat, so there is a higher risk of getting cancer for women with dense breasts. Density level 4 women have five times the cancer risk as a density level 1". (NEJM)http://www.huffingtonpost.com/nikki-weissgoldstein/breast-density_b_5908410.html, 2014.)
FOLLOWING UP MAMMOGRAMS WITH ULTRASOUND FOR WOMEN WITH DENSE BREASTS - MORE ABOUT THE BREAST DENSITY NOTIFICATION LAW
While the American Cancer Society does not recommend an ultrasound in place of a mammogram, there is a concession that, " ...Clinical trials are now looking at the benefits and risks of adding breast ultrasound to screening mammograms in women with dense breasts and a higher risk of cancer". (www.cancer.org/cancer/breastcancer/detailedguide/breast-cancer-diagnosis.)
Indeed, if a woman is found to have dense breasts on a mammogram, as of July 2015, in 24 states so far, a breast density notification law mandates that a letter be sent to the woman informing that she has dense breasts. "The intent of such a law was to give women the necessary information to decide on further action if they had dense breast tissue. Dense breast tissue makes it harder to identify cancer on a mammogram and may also be associated with an increased risk of breast cancer, according to the American College of Radiology. Women with dense breasts are encouraged to discuss with their physicians their possible increased risk of breast cancer and the difficulty that mammography may have in detecting tumors."
Time for further testing! How about an ultrasound, which is helpful in dense breast imaging? While Connecticut passed the first breast density notification law in 2009, many, many states have followed, such as California, New York, and Pennsylvania. CHECK THE MAP ABOVE. http://www.diagnosticimaging.com/breast-imaging/breast-density-notification-laws-state-interactive-map#sthash.nXIJf0Q9.dpuf.
ULTRAOUNDS INSTEAD OF MAMMOGRAMS?
EDITORS' NOTE
Since an ultrasound does NOT use radiation, especially if you are younger and have dense breasts, you may wish to consider getting an ultrasound in lieu of a mammogram. However, different hospitals and different insurance companies have their own rules for screening protocols., mostly favoring mammograms. Nevertheless, it is always worth a concerted effort to try to get an ultrasound if you do not wish to have a mammogram.
EDITORS' NOTE
Since an ultrasound does NOT use radiation, especially if you are younger and have dense breasts, you may wish to consider getting an ultrasound in lieu of a mammogram. However, different hospitals and different insurance companies have their own rules for screening protocols., mostly favoring mammograms. Nevertheless, it is always worth a concerted effort to try to get an ultrasound if you do not wish to have a mammogram.
SO, YOU HAVE CHOSEN TO HAVE AN ULTRASOUND. WHAT IS AN ULTRASOUND? DEFINITION
"Ultrasound, also known as sonography, uses sound waves to outline a part of the body. For this test, a small, microphone-like instrument called a transducer, is placed on the skin (which is often first lubricated with ultrasound gel). It emits sound waves and picks up the echoes as they bounce off body tissues. The echoes are converted by a computer into a black and white image that is displayed on a computer screen. This test is painless and does not expose you to radiation. (No radiation!) Ultrasound has become a valuable tool to use along with mammography because it is widely available and less expensive than other options, such as MRI. Usually, breast ultrasound is used to target a specific area of concern found on the mammogram."
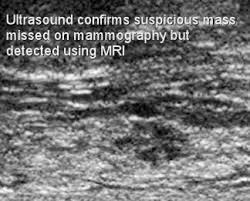
Note that ultrasounds are generally thought to be a second-look, to see if a problem area on a mammogram is a solid (tumor) or liquid (fluid-filled cyst).
"Ultrasound helps distinguish between cysts (fluid-filled sacs) and solid masses and sometimes can help tell the difference between benign and cancerous tumors. In someone with a breast tumor, it can also be used to look for enlarged lymph nodes under the arm." (www.cancer.org/cancer/breastcancer/detailedguide/breast-cancer-diagnosis.)
BREAST IMAGING- ULTRASOUNDS
WHICH BETTER DETECTS THE SIZE OF THE TUMOR -
MAMMOGRAMS, MRI, OR ULTRASOUND?
"We found that in patients who underwent lumpectomy after breast cancer
was visualized preoperatively on all three imaging modalities,
ultraound performed better than mammogram and MRI for preoperative tumor size measurement,
and overall tumor staging.".
was visualized preoperatively on all three imaging modalities,
ultraound performed better than mammogram and MRI for preoperative tumor size measurement,
and overall tumor staging.".
Ultrasounds! .... According to a 2015 study, " ... Ultrasound measurements being slightly more accurate than mammogram measurements".
In the Leddy R et al. 2015 study, the researchers sought to compare the accuracy of the tumor size via mammograms, MRIs, or ultrasounds.
For their study, "Records from patients who underwent breast cancer lumpectomy between 2008 and 2012 and in whom tumor was seen on all three imaging modalities were retrospectively reviewed for maximum tumor size measurements."
Conclusion: "Preoperative MRI significantly overestimated tumor size. Measurements obtained on ultrasounds and mammograms were more accurate irrespective of breast density, with ultrasound measurements being slightly more accurate than mammogram measurements."
(See Leddy R et al., Comparative Accuracy of Preoperative Tumor Size Assessment on Mammography, Sonography, and MRI: Is the Accuracy Affected by Breast Density or Cancer Subtype?", J Clin Ultrasound, 2015.)
BREAST IMAGING - ULTRASOUNDS
YOUNG? DENSE BREASTS? HIGH RISK FOR BREAST CANCER?
ULTRASOUND SUPERIOR TO MAMMOGRAMS IN HIGH-RISK CHINESE WOMEN
In the Shen S et al. 2015 study, the researchers evaluated both the cost and effectiveness of ultrasounds as opposed to mammograms in high-risk Chinese women.
High-risk Chinese women were screened either by "mammography alone, ultrasound alone, or by both methods at the time of enrollment in the study and at one year follow-up".
Results: "Among the 30 cancers (of which 15 were stage0/1) detected, 5 were in the mammography group, 11 in the ultrasound group, and 14 in the combined group. In the combined group, ultrasound detected all the 14 cancers, whereas mammography detected 8, making ultrasound more sensitive with a better diagnostic accuracy."
Why did ultrasounds prove to be more effective? "We attribute the low sensitivity of mammography in this study mainly to the effects of younger age of the study population with a mean age of 46 years and 68% of the women were premenopausal who are more likely to have denser breast tissue. Chinese women are commonly found to have dense breasts, with 66% classified as heterogeneous or extremely dense. ... Although age hardly affects the ultrasound exam, mammography appears to be more sensitive for patients over 50 years of age than those younger."
Conclusion: "Ultrasound is superior to mammography for breast cancer screening in high-risk Chinese women." Note, in addition, that ultraound offers a lower cost and is a more acceptable testing procedure."(See Shen S et al., A Multi-Center Randomized Trial Comparing Ultrasound Versus Mammography for Screening Breast Cancer in High-Risk Chinese Women, British Medical Journal, 2015.)
BREAST IMAGING - ULTRASOUNDS
ULTRASOUNDS FOLLOWING NEGATIVE MAMMOGRAMS
4.6 ADDITIONAL CANCERS FOUND AMONG 1000 WOMEN WITH NEGATIVE MAMMOGRAMS.
In the Hwang J-Y et al. 2015 study, the researchers sought to determine if an ultrasound exam following a negative mammogram might pick up additional cancers.
Among 1727 women, from ages 30-76 (median 49.5 years), 78.1% had dense breasts on their mammograms, making the ultrasound an ideal test to find additional problems.
Conclusion: "Our study shows that screening ultrasound detected 4.6 additional cancers among 1000 women with negative mammography, a 4.3% rate of probable benign findings, and a 5.8% recall rate in the population, 44.1% of whom had previous breast ultrasound." Note that, "The recall rate was 5.8%, which is in lower bound of acceptable range of mammography (5-12%), according to American College of Radiology standard." (See Hwang J-Y et al., Screening Ultrasound in Women with Negative Mammography: Outcome Analysis, Yonsei Med J, 2015.)
IMAGING
THERMOGRAMS
THERMOGRAMS CAN NOT DEFINITIVELY FIND BREAST CANCER
EDITORS' NOTE
As this THERMOGRAMS' section illustrates, thermography is NOT definitive for a diagnosis of breast cancer. However, thermograms may be useful to pick up signs of temperature change that may be indicative of pre-cancerous issues that will give a woman the opportunity to take steps to remedy these aberrant changes.
EDITORS' NOTE
As this THERMOGRAMS' section illustrates, thermography is NOT definitive for a diagnosis of breast cancer. However, thermograms may be useful to pick up signs of temperature change that may be indicative of pre-cancerous issues that will give a woman the opportunity to take steps to remedy these aberrant changes.
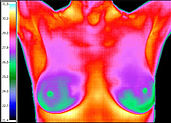
NORMAL THERMOGRAM!
BASED ON A CLASSIFICATION SYSTEM (TH-1 - TH-6), THIS NORMAL THERMOGRAM IS
TH-1.
BASED ON A CLASSIFICATION SYSTEM (TH-1 - TH-6), THIS NORMAL THERMOGRAM IS
TH-1.
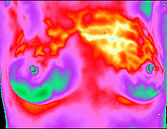
ABNORMAL THERMOGRAM!
BASED ON A CLASSIFICATION SYSTEM, THIS ABNORMAL THERMOGRAM
IS TH-5, DEPICTING VERY HIGH RISK FOR BREAST CANCER>
BASED ON A CLASSIFICATION SYSTEM, THIS ABNORMAL THERMOGRAM
IS TH-5, DEPICTING VERY HIGH RISK FOR BREAST CANCER>
"The sensitivity of thermography in breast cancer detection is low and the evidence does not support thermography as an alternative to screening mammography or for the investigation of symptoms." Meagan Brennan and Nehmat Houssami, 2013.
"Thermography cannot be proclaimed as a screening method, without any evidence whatsoever." Brkljacic B et al., 2013..
" Thermograms may be useful for clarifying the significance of an abnormal mammogram or for adjunctive imaging of a highly suspicious palpated mass. However, the clinician needs to be prepared to translate the accuracy statistics for the patient and to carefully document informed consent in the event that the patient chooses to forego biopsy of a breast mass. ....There are other applications that might be more appropriate for thermograms that this article did not measure. These uses include the detection of precancerous dysplasia, the accurate assessment of long-term risk of developing breast cancer, and the evaluation of possible dysplasia developing in response to hormone replacement therapy." See Katherine Neubauer, ND, Are Breast Thermograms Enough to Use?, Natural Medicine Journal, 2011.
" We presented results that were carefully analyzed and shown as a new insight in the existing area: use of mammography and thermography simultaneously. We confirmed the high sensitivity of thermography, and based on other similar research, we concluded that 'it would be prudent' (no must or have to ) 'to use thermography as a primary screening method' (not the only one) 'in detection of breast carcinomas'." Darko Kolaric and Iskra Nola, Reply on "Thermography is Not a Feasible Method for Breast Cancer Screenings" By Brkljacic et al., Coll Anthropol, 2015.)
WHAT IS THERMOGRAPHY?
"The use of Digital Infrared Imaging (DII thermography) is based on the principle that metabolic activity and vascular circulation in both pre-cancerous tissue and the area surrounding a developing breast cancer is almost always higher than in normal breast tissue.
In an ever-increasing need for nutrients, cancerous tumors increase circulation to their cells by holding open existing blood vessels, opening dormant vessels, and creating new ones (neoangiogenesis). This process frequently results in an increase in regional surface temperatures of the breast. DII uses ultra-sensitive medical infrared cameras and sophisticated computers to detect, analyze, and produce high-resolution images of these temperature variations. Because of DII’s extreme sensitivity, these temperature variations may be among the earliest signs of breast cancer and/or a pre-cancerous state of the breast.
DII’s ability to detect thermal signs that may suggest a pre-cancerous state of the breast, or signs of cancer at an extremely early stage, lies in its unique capability of monitoring the temperature variations produced by the earliest changes in tissue physiology (function). However, DII does not have the ability to pinpoint the location of a tumor nor can it detect 100% of all cancers. Consequently, Digital Infrared Imaging’s role is in addition (an adjunct) to mammography and physical examination, not in lieu of. DII does not replace mammography, and mammography does not replace DII; the tests complement each other." (See http://www.breastthermography.com/breast_thermography_mf.htm,)
BREAST IMAGING - THERMOGRAMS
2015 STUDY COMPARING DIAGNOSED TUMORS TO THERMOGRAM STUDIES
MORE AGGRESSIVE TUMORS SHOW INCREASED TEMPERATURES
THERMOGRAM TEMPERATURE STUDIES OF BREAST TUMORS
Average temperature of the tumor (C)
Hormone positive - 34.58
Hormone negative - 34.95
HER2 + (positive) - 35.18
"The results revealed that positive HER-2 tumors had the highest impact on the increased temperature. The HER-2 belongs to a family of the 4 transmembrane receptor tyrosine kinases that mediate the growth, differentiation, and survival rate of cells. It is overexpressed or amplified in approximately 15–25% of breast cancers, and it has been associated with aggressive tumor behavior." Zore C et al., 2015
Average temperature of the tumor (C)
Hormone positive - 34.58
Hormone negative - 34.95
HER2 + (positive) - 35.18
"The results revealed that positive HER-2 tumors had the highest impact on the increased temperature. The HER-2 belongs to a family of the 4 transmembrane receptor tyrosine kinases that mediate the growth, differentiation, and survival rate of cells. It is overexpressed or amplified in approximately 15–25% of breast cancers, and it has been associated with aggressive tumor behavior." Zore C et al., 2015
What is the relationship between thermograms and diagnosed breast cancer tumors? In the Zore Z et al. 2015 experiment, thermograms were conducted on already diagnosed breast cancer patients prior to surgery.
Results:
*Increased temperatures on the thermograms were more dependent on the IHC (showing receptors, such as hormone receptors and HER2 receptors)..
*Temperatures were the coldest for the hormone positive tumors ( HER2 negative) and more amenable to treatment.
*Temperatures were the warmest for the tumors that are estrogen positive, progesterone negative, HER2 positive, and have a high proliferative Ki rate that are more difficult to treat.
*Tumor size is irrelevant for temperatures.
Conclusion: "Statistically significant difference of thermographic findings between healthy and affected breast was found for positive human epidermal growth factor receptor-2 (HER-2) tumors, negative progesterone receptors (PR−) and a high proliferative activity (Ki)..." (See Zore Z et al., Association of Clinical, Histopathological and Immunohistochemical Prognostic Factors of Invasive Breast Tumors and Thermographic Findings, Infrared Physics and Technology, 2015.)
BREAST IMAGING - THERMOGRAMS
THERMOGRAM SENSITIVITY FOR BREAST CANCER IS LOW
In 2013, Brennan and Houssami reviewed the literature on thermograms to assess thermography's efficacy in finding breast cancer.
Review Results: Out of seventeen studies, four studies reported median sensitivity to finding breast cancer (47% with a range of 25–70%) and the median false-positive rate was 31% (range 21–38%). "Twelve studies reported thermography accuracy (9887 women) in the context of a known clinical or mammographic abnormality: median sensitivity was 59% (range 25–97%). Two studies found no association between abnormal thermography and an increased 5-year risk of developing breast cancer."
Conclusion: "The sensitivity of thermography in breast cancer detection is low and the evidence does not support thermography as an alternative to screening mammography or for the investigation of symptoms." (See Brennan M and Houssami N, Thermography in Breast Cancer Diagnosis, Screening, and Risk Assessment Systemic Review, Breast Cancer Management, 2013.)
BREAST IMAGING - THERMOGRAMS
IS THERMOGRAPHY A "FEASIBLE" METHOD TO SCREEN FOR BREAST CANCER?
Yes!...... According to the Kolaric D et al. 2013 study finding thermograms can be used as a breast cancer imaging modality.
For their study, "Ultrasounds, mammograms, and thermograms were done on 26 patients slated for breast cancer surgery. For the thermograms, "Thermographic imaging was performed using a new generation of digital thermal cameras with high sensitivity and resolution."
Findings: " While mammography detected 31 changes in 26 patients, thermography was more sensitive and detected 6 more changes in the same patients. All 37 changes were subjected to the cytological analysis and it was found that 16 of samples were malignant, 8 were suspected malignant and 11 were benign with atypia or proliferation while only 2 samples had benign findings.... Statistical analysis of the data has shown a probability of a correct mammographic finding in 85% of the cases (sensitivity of 85%, specificity of 84%) and a probability of a correct thermographic finding in 92% of the cases (sensitivity of 100%, specificity of 79%)."
Conclusion: " ... We believe that thermography should immediately find its place in the screening programs for early detection of breast carcinoma, in order to reduce the sufferings from this devastating disease." (See Kolaric D et al., Thermography -- A Feasible Method For Screening Breast Cancer?, Coll Antropol, 2013.) Editors' Note: See below for a dissenting opinion.
BREAST IMAGING- THERMOGRAMS
IS THERMOGRAPHY A "FEASIBLE" METHOD TO SCREEN FOR BREAST CANCER?
A DISSENTING OPINION
No! ..... According to the Brkljacic B et al. 2013 study, there is no evidence supporting thermography.
Here is their criticism of the Kolaric study cited just above:"The conclusion that thermography might be feasible for screening cannot be derived from studies with small sample size, unclear selection of patients, and in which mammography and thermography were not blindly compared as screening modalities. Thermography can not be used to aspirate, biopsy or localize lesions preoperatively since no method so far was described to accurately transpose the thermographic location of the lesion to the mammogram or ultrasound and to surgical specimen. Thermography cannot be proclaimed as a screening method, without any evidence whatsoever." (See Brklijacic B et al., Thermography is Not a Feasible Method for Breast Cancer Screening, Coll Antropol, 2013.)