HERBS AND SUPPLEMENTS
" 'We discovered that while the parasite (Theileria) is living inside the white blood cell it secretes a special protein, called Pin1. This protein is then able to 'mess around' with the cell and trigger mechanisms which control cell behaviour -so it starts acting like a cancer cell." And, in addition, " 'We also found that an anti-parasite drug can target this protein and reverse the cancer-like state. This is an exciting example of how parasites hijack the host cell and how these parasite proteins can be targeted by drugs. It also directly links a parasite protein to cancer-causing cell processes, giving us a real insight into how infection with parasites and other organisms might lead to cancer in humans.' "
Professor Jonathan Weitzman, Marsolier J et al., 2015.
Professor Jonathan Weitzman, Marsolier J et al., 2015.
In this study, "Pin1 is directly inhibited by the anti-parasite drug, buparvaquone (and other known PIN1 inhibitors)."
Compellingly, another such Pin1 inhibitor is JUGLONE, which is found in the anti-parasite herb, black walnut. In the Kanoaka R et al. 2015 study, the Pin1 inhibitor, juglone, was able to exert anti-cancer activities against prostate cancer cells.
HOW ABOUT SOME ANTI-PARASITE HERBS, SUCH AS BLACK WALNUT? READ THIS SECTION FOR MORE INFO.
Special thanks to M.W., a member of Breast Cancer Study and Support, for compiling research on Pin1 and juglone.
Compellingly, another such Pin1 inhibitor is JUGLONE, which is found in the anti-parasite herb, black walnut. In the Kanoaka R et al. 2015 study, the Pin1 inhibitor, juglone, was able to exert anti-cancer activities against prostate cancer cells.
HOW ABOUT SOME ANTI-PARASITE HERBS, SUCH AS BLACK WALNUT? READ THIS SECTION FOR MORE INFO.
Special thanks to M.W., a member of Breast Cancer Study and Support, for compiling research on Pin1 and juglone.
"The art of healing comes from nature, not from the physician. Therefore, the physician must start from nature with an open mind."
Paracelsus.
"It is worthwhile to start using natural and prescribed antibiotics, anti-fungal, and anti-parasitic medications, as a means to reduce the total burden of infections, as a part of cancer management programs by primary care physicians. It may have a secondary benefit of targeting the mitochondria of cancer stem cells ... "
Simon Yu, MD, www.preventionandhealing.com/articles/Cancer-Infectious-Disease-Metabolic-Parasites-Biology-Cancer-Cells.pdf?utm_source=Email+Newsletter+-+201504+%2395&utm_campaign=Newsletter+April+2015&utm_medium=email
CLOVES, WORMWOOD, BLACK WALNUT, AND DIGESTIVE ENZYMES - ALL HAVE ANTI-CANCER PROPERTIES. ALSO, THE HERBS AND DIGESTIVE ENZYMES CONSTITUTE AN EXAMPLE OF AN ANTI-PARASITE CLEANSE. SINCE ALL THESE HERBS AND THE DIGESTIVE ENZYMES HAVE ANTI-CANCER PROPERTIES, DOES THE KILLING OF PARASITES FACTOR INTO THEIR ANTI-CANCER EFFICACY?
(If you would like to consider Dr. Clark's herbal formula of cloves, wormwood, black walnut, and digestive enzymes, go to: http://www.drclark.net/en/cleanses/beginners/herbal-parasite-cleanse.)
PARASITES AND CANCER - WHY WE NEED ANTI-PARASITE HERBS TO RID BUGS
"Carcinogenesis associated with helminth (parasitic worm) infections is a complex process, which may involve several different mechanisms, but chronic inflammation is a key feature. Host immune responses and immunopatholgical processes mediate inflammatory responses and any failure in the control of the immunological components involved in this response can lead to chronic inflammation. .... Inflammatory cells generate free radicals and nitrogen species, which can oxidize and damage DNA and lead to genetic instabilities and malignant transformation. Physical damage caused by the parasites, their eggs or secreted products leads to restorative hyperplasia of the damaged tissue.... "
(See Vennervald BJ et al., Helminths and Malignancy, Parasite Immunol, 2009.)
A PARASITE AND CANCER-LIKE CELLS - 2015 RESEARCH: HOW ANTI-PARASITE HERBS HELPED REVERSE CANCER- LIKE CELLS
From Science Daily:
"Scientists have pinned down how a dangerous tropical parasite which is transmitted by ticks manages to turn healthy cells into cancer-like invasive cells, according to research. Microscopic Theileria parasites infect the blood of mammals, particularly cattle, causing serious illness."
The parasite infects white blood cells....
The parasite can infect the white blood cells and make them behave cancer-like. The lead researcher, Professor Jonathan Weitzman said, "We discovered that while the parasite is living inside the white blood cell it secretes a special protein, called Pin1. This protein is then able to 'mess around' with the cell and trigger mechanisms which control cell behaviour -so it starts acting like a cancer cell." And, in addition, "We also found that an anti-parasite drug can target this protein and reverse the cancer-like state. This is an exciting example of how parasites hijack the host cell and how these parasite proteins can be targeted by drugs. It also directly links a parasite protein to cancer-causing cell processes, giving us a real insight into how infection with parasites and other organisms might lead to cancer in humans."
(See Science Daily,http://www.sciencedaily.com/releases/2015/01/150126112243.htm. For the study, see Marsolier J et al., Theileria Parasites Secrete a Prolyl Isomerase to Maintain Host Leukocyte Transformation, Nature, 2015.)
THE HERB, CLOVES
"Syzygium aromaticum (clove) ranks highest in terms of antioxidant properties, followed by cinnamon, pepper, ginger, and garlic."
Kumar P et al., 2014.
CLOVES AND HEALTH BENEFITS
The herb, cloves (Syzgium Aromaticum), has many health benefits. "Traditional uses in America include treating worms, viruses, candida, various bacterial and protozoan infections. Laboratory tests on cloves identify eugenol as being the possible reason for the antimibrocial actions, and confirm cloves' effectiveness in inhibiting food-borne pathogens as well as other bacteria and fungi. The volatile oil of cloves (about 85-90% eugenol) was highly active against a range of test microorganisms, being classified as bactericidal in nature."
Bhowmik D et al., Recent Trends in Indian Traditional Herbs Syzgium Aromaticum and its Health Benefits, J Pharmacognosy and Phyochemistry, 2012.
CLOVES' ANTHELMINTIC ACTIVITY AGAINST EARTHWORMS
In a 2015 review article, Kumar P et al. explored the effects of aqueous extracts of cloves against earthworms, specifically the Indian earthworm, Pheritma posthuma.
The researchers found that in killing the earthworms, there was a "dose dependent paralyzing and death in the earthworms. Higher concentrations of extract product produced a paralytic effects much earlier and the time taken for death was shorter for all worms. Phytochemical screening of crude extracts revealed the presence of tannins which are shown to have anthelmintic activity."
(See Kumar P et al., In Vitro Anthelmintic Activity of Syzgium Aromaticum Floral Buds and Cinnamomum Zeylanicum Bark Aqueous Extracts, Int J Pharm Bio Sci, 2015.)
CLOVES' BACTERIAL EFFECT - STRONG ANTIMICROBIAL ACTIVITY?
Yes!
In the 2008 Saeed and Tariq study, the researchers "investigated the potential of using aqueous infusion, decoction and essential oil of cloves as natural antibacterial agents" against gram negative bacteria.
Results? " Essential oil of clove exhibited maximum activity against V. cholerae with 23.75 mm mean diameter of zone of inhibition plus minus 3.03 standard deviation. K. ozaenae, K. pneumoniae, S. marcescens, S. typhi, S. dysentriae and V. cholerae were found resistant to aqueous infusion and decoction while essential oil showed strong antibacterial activity against all bacterial isolates tested."
(See Saeed and Tariq, In Vitro Antibacterial Activity of Clove Against Gram Negative Bacteria, Food and Agriculture Organization of the United Nations, 2008.)
EUGENOL (IN CLOVES) INHIBITS TOXIN (DMBA) GENOTOXICITY IN BREAST CANCER CELLS
Can eugenol, in cloves, be a chemopreventive agent?
Yes!
There are two ways that a toxin can be detoxified: Either the CYP enzymes (CYP450s) promoting the toxins are inhibited, or the phase II detoxifying enzymes are induced.
What was the effect of eugenol on the DMBA toxin-induced DNA damage in breast cancer cells?
Not only did eugenol "inhibit the formation of the DMBA-DNA adduct" via inhibition of CYP1A1 and CYP1B1 activity, but there was an increase in "NAD(P)H:quinone oxidoreductase (QR), a major detoxifying enzyme for DMBA through NF-E2 related factor2 binding to antioxidant response element in QR gene."
Conclusion: Eugenol in cloves has a "potential" to prevent harm from the toxin, DMBA, both through suppressing its activation and in promoting its detoxification.
(See Eun H et al., Eugenol Inhibit 7,12-dimethylbenz{a] anthracene-Induced Genotoxicity in MCF-7 Cells: Bifunctional Effects on CYP1 and NADPH: Quinone Oxidoreductase, Federation of European Biochemical Societies, 2007.)
CYTOTOXIC EFFECTS OF CLOVES IN BREAST CANCER CELLS
In the Kumar P et al. 2014 study, researchers investigated both in the test tube and in humans what "bioactive compounds are responsible for its (cloves) antitumor activity."aims to evaluate the cytotoxic activity of cloves toward MCF-7 human breast cancer cell lines."
From cloves, a water extract, ethanol extract, and essential oil of cloves were used in "different concentrations" to test their potential to kill breast cancer cells.
Results? "When both extracts were incubated at a higher concentration or for a longer period of 48 hours, the IC50 (inhibitory) values of the ethanol extract and essential oil became much lower compared with those at 24 hours of incubation. This suggests that the ethanol extract and essential oil of cloves inhibit the MCF-7 human breast cancer cell lines in a time- and dose-dependent manner."
(See Kumar P et al., Anticancer Potential of Syzygium Aromaticum L. in MCF-7 Human Breast Cancer Cell Lines, Pharmacognosy Res, 2014.)
SOME REASONS WHY CLOVES MAY BE EFFECTIVE AGAINST BREAST CANCER CELLS AND OTHER CANCER CELLS
In the 2014 Liu H et al. study, the researchers "investigated the in vitro and in vivo antitumor effects and biological mechanisms of ethyl acetate extract of cloves (EAEC) and the potential bioactive components responsible for its antitumor activity." The in vitro tests were conducted on many different cancers, including breast cancer cells.
In both in vitro and in vivo experiments, the researchers found that "oleanolic acid (OA)" was one of the components of the cloves extract that was "responsible for its antitumor activity." It should be noted that both oleanolic acid and the extract of cloves were cytotoxic against several different cancer cell types.
In vitro, the extract's antiproliferative activity was "likely mediated by oleanolic acid".
However, in vivo, they found that this extract was superior to oleanolic acid and the chemo drug 5-fluorouracil "at suppressing the growth of colon cancer xenografts". Import? "This suggests that either additional components of the extract may play a role in its in vivo activity or that absorption and metabolism influence its antitumor ability."
Summary: "Our studies have shown that the ethyl acetate extract of cloves displayed antitumor activity both in vitro and in vivo. Clove extract may represent a novel therapeutic herb for cancer treatment, and oleanolic acid is one of the components responsible for part of its antitumor activity."
(See Liu H et al., Clove Extract Inhibits Tumor Growth and Promotes Cell Cycle Arrest and OptoptosisOncol Res, 2014.)
Kumar P et al., 2014.
CLOVES AND HEALTH BENEFITS
The herb, cloves (Syzgium Aromaticum), has many health benefits. "Traditional uses in America include treating worms, viruses, candida, various bacterial and protozoan infections. Laboratory tests on cloves identify eugenol as being the possible reason for the antimibrocial actions, and confirm cloves' effectiveness in inhibiting food-borne pathogens as well as other bacteria and fungi. The volatile oil of cloves (about 85-90% eugenol) was highly active against a range of test microorganisms, being classified as bactericidal in nature."
Bhowmik D et al., Recent Trends in Indian Traditional Herbs Syzgium Aromaticum and its Health Benefits, J Pharmacognosy and Phyochemistry, 2012.
CLOVES' ANTHELMINTIC ACTIVITY AGAINST EARTHWORMS
In a 2015 review article, Kumar P et al. explored the effects of aqueous extracts of cloves against earthworms, specifically the Indian earthworm, Pheritma posthuma.
The researchers found that in killing the earthworms, there was a "dose dependent paralyzing and death in the earthworms. Higher concentrations of extract product produced a paralytic effects much earlier and the time taken for death was shorter for all worms. Phytochemical screening of crude extracts revealed the presence of tannins which are shown to have anthelmintic activity."
(See Kumar P et al., In Vitro Anthelmintic Activity of Syzgium Aromaticum Floral Buds and Cinnamomum Zeylanicum Bark Aqueous Extracts, Int J Pharm Bio Sci, 2015.)
CLOVES' BACTERIAL EFFECT - STRONG ANTIMICROBIAL ACTIVITY?
Yes!
In the 2008 Saeed and Tariq study, the researchers "investigated the potential of using aqueous infusion, decoction and essential oil of cloves as natural antibacterial agents" against gram negative bacteria.
Results? " Essential oil of clove exhibited maximum activity against V. cholerae with 23.75 mm mean diameter of zone of inhibition plus minus 3.03 standard deviation. K. ozaenae, K. pneumoniae, S. marcescens, S. typhi, S. dysentriae and V. cholerae were found resistant to aqueous infusion and decoction while essential oil showed strong antibacterial activity against all bacterial isolates tested."
(See Saeed and Tariq, In Vitro Antibacterial Activity of Clove Against Gram Negative Bacteria, Food and Agriculture Organization of the United Nations, 2008.)
EUGENOL (IN CLOVES) INHIBITS TOXIN (DMBA) GENOTOXICITY IN BREAST CANCER CELLS
Can eugenol, in cloves, be a chemopreventive agent?
Yes!
There are two ways that a toxin can be detoxified: Either the CYP enzymes (CYP450s) promoting the toxins are inhibited, or the phase II detoxifying enzymes are induced.
What was the effect of eugenol on the DMBA toxin-induced DNA damage in breast cancer cells?
Not only did eugenol "inhibit the formation of the DMBA-DNA adduct" via inhibition of CYP1A1 and CYP1B1 activity, but there was an increase in "NAD(P)H:quinone oxidoreductase (QR), a major detoxifying enzyme for DMBA through NF-E2 related factor2 binding to antioxidant response element in QR gene."
Conclusion: Eugenol in cloves has a "potential" to prevent harm from the toxin, DMBA, both through suppressing its activation and in promoting its detoxification.
(See Eun H et al., Eugenol Inhibit 7,12-dimethylbenz{a] anthracene-Induced Genotoxicity in MCF-7 Cells: Bifunctional Effects on CYP1 and NADPH: Quinone Oxidoreductase, Federation of European Biochemical Societies, 2007.)
CYTOTOXIC EFFECTS OF CLOVES IN BREAST CANCER CELLS
In the Kumar P et al. 2014 study, researchers investigated both in the test tube and in humans what "bioactive compounds are responsible for its (cloves) antitumor activity."aims to evaluate the cytotoxic activity of cloves toward MCF-7 human breast cancer cell lines."
From cloves, a water extract, ethanol extract, and essential oil of cloves were used in "different concentrations" to test their potential to kill breast cancer cells.
Results? "When both extracts were incubated at a higher concentration or for a longer period of 48 hours, the IC50 (inhibitory) values of the ethanol extract and essential oil became much lower compared with those at 24 hours of incubation. This suggests that the ethanol extract and essential oil of cloves inhibit the MCF-7 human breast cancer cell lines in a time- and dose-dependent manner."
(See Kumar P et al., Anticancer Potential of Syzygium Aromaticum L. in MCF-7 Human Breast Cancer Cell Lines, Pharmacognosy Res, 2014.)
SOME REASONS WHY CLOVES MAY BE EFFECTIVE AGAINST BREAST CANCER CELLS AND OTHER CANCER CELLS
In the 2014 Liu H et al. study, the researchers "investigated the in vitro and in vivo antitumor effects and biological mechanisms of ethyl acetate extract of cloves (EAEC) and the potential bioactive components responsible for its antitumor activity." The in vitro tests were conducted on many different cancers, including breast cancer cells.
In both in vitro and in vivo experiments, the researchers found that "oleanolic acid (OA)" was one of the components of the cloves extract that was "responsible for its antitumor activity." It should be noted that both oleanolic acid and the extract of cloves were cytotoxic against several different cancer cell types.
In vitro, the extract's antiproliferative activity was "likely mediated by oleanolic acid".
However, in vivo, they found that this extract was superior to oleanolic acid and the chemo drug 5-fluorouracil "at suppressing the growth of colon cancer xenografts". Import? "This suggests that either additional components of the extract may play a role in its in vivo activity or that absorption and metabolism influence its antitumor ability."
Summary: "Our studies have shown that the ethyl acetate extract of cloves displayed antitumor activity both in vitro and in vivo. Clove extract may represent a novel therapeutic herb for cancer treatment, and oleanolic acid is one of the components responsible for part of its antitumor activity."
(See Liu H et al., Clove Extract Inhibits Tumor Growth and Promotes Cell Cycle Arrest and OptoptosisOncol Res, 2014.)
THE HERB, WORMWOOD
There are different varieties of wormwood. A derivative of the sweet wormwood variety, Artemisia annua, is artemisinin. Artemisinin is used in research due to its bioactivity, the conformity in dosage, and a profit motive. Also please note that artesunate, a patented pharmaceutical drug (a semi-synthetic derivative of artemisinin), is also being used. Since the whole herb has all of the known components plus many undiscovered ones, not to mention that the extraction process may involve solvents, etc., the EDITORS strongly recommend that the reader always consider ONLY taking the whole herb. TAKE WORMWOOD.)
BREAST CANCER STRATEGY
Artemisia absinthium (wormwood) was able to inhibit both estrogen-positive and estrogen-negative breast cancer cells via 'the induction of apoptosis by regulating Bcl-2 family proteins and MEK/MAPK signaling'.
Gowhar S et al., 2012 READ FURTHER DOWN FOR COMMENTS ON THE STUDY.
WORMWOOD BACKGROUND
"It (wormwood) is used in indigenous medicine as a vermifuge, an insecticide, an antispasmodic, an antiseptic, and in the treatment of chronic fever and inflammation of the liver. Its essential oil has antimicrobial and antifungal activity. Chemical analysis of Artemisia Absinthium extracts has shown that its volatile oil is rich in thujone, which has been reported as an anthelmintic."
(See Gowhar S et al., Artemisia Absinithium : A Novel Potential Complementary and Alternative Medicine for Breast Cancer, Molecular Biology Reports, 2012
WORMWOOD KILLS THE MALARIA PARASITE, BUT WORMWOOD GOES BEYOND THE DISEASE OF MALARIA
Ho We et al., in their 2013 study. describe artemisins: "Artemisinins are a family of sesquiterpene trioxane lactone anti-malarial agents originally derived from Artemesia annua L. The anti-malarial action of artemisins involves the formation of free radicals via cleavage of the endoperoxide bond in its structure, which mediate eradication of the Plasmodium species."
Explanation? The Plasmodium malaria parasite, due to its living in the red blood cell, has a high amount of iron. And artemisinin loves a rich iron environment. When artemisinin, with its double oxygen bond, comes into contact with all of that iron, free radicals are formed, and the parasite is harmed.
The researchers argue that artemisinins have a value in other actions besides malaria. While it is known that artemisinin as wormwood is able to kill WORMS, "Artemisinins have been reported to possess robust inhibitory effects against viruses (e.g. Human cytomegalovirus), protozoa (e.g. Toxoplasma gondii), helminths (e.g. Schistosoma species and Fasciola hepatica) and fungi (e.g. Cryptococcus neoformans). Artemisinins have demonstrated cytotoxic effects against a variety of cancer cells by inducing cell cycle arrest, promoting apoptosis, preventing angiogenesis, and abrogating cancer invasion and metastasis. Artemisinins have been evaluated in animal models of autoimmune diseases, allergic disorders and septic inflammation."
(See Ho We et al., Artemisinins: Pharmacological Actions Beyond Anti-Malarial, Pharmacol Ther, 2013.)
ARTEMISININS AND BREAST CANCER - EXPLOITING THE IRON RICH ENVIRONMENT OF CANCER CELLS
Drawing from artemisinin's success with malaria, Dr. Henry Lai reasoned that cancer cells, with their "significantly more intracellular iron" (cancer cells use more iron to replicate) would succumb to the artemisinin, just like the malaria parasite.
Again, the artemisinin treatment is just like an oxidative therapy. After all, there is a peroxide linkage, as the two oxygen atoms are linked together, and any peroxide that meets up with iron creates free radicals and consequential damage. According to Dr. Lai et al., artemesia "is selectively more toxic to cancer than normal cells" due to the high iron content. Already these researchers had found that when artemisinin is tagged with transferrin (iron-carrying), it "enhanced the selectivity and toxicity of artemisinin toward cancer cells in vitro." Note that, in this case, almost all of the breast cancer cells were killed.
But that's just cells in a petri dish. What about in an animal model?
In a rat model of breast cancer, breast cancer was induced from cancer cells. Once the tumors appeared, there were daily injections of artemisinin-transferrin conjugate. Results? "The conjugate significantly retarded the growth rate of breast tumors in the rat." No significant side effect was observed in the rats during treatment.
(See Lai H et al., Artemisinin-Transferrin Conjugate Retards Growth of Breast Tumors in the Rat, Anticancer Research, 2009.)
CAN ARTEMISININ DELAY THE DMBA TOXIN FROM CAUSING BREAST CANCER IN RATS?
Yes!
In another Dr. Henry Lai study, the day after an oral injection of "dimethylbenz[a]anthracene (DMBA), known to induce multiple breast tumors" in rats, "one group of rats was provided with a powdered rat-chow containing 0.02% artemisinin, whereas a control group was provided with plain powdered food. For 40 days, the rats were watched for signs of tumor formation.
Results? "Oral artemisinin significantly delayed and in some animals prevented (57% of artemisinin-fed versus 96% of the controls developed tumors, breast cancer development in the monitoring period. In addition, breast tumors in artemisinin-fed rats were significantly fewer and smaller in size when compared with controls."
(See Lai H et al., Oral Artmisinin Prevents and Delays the Development of 7,12 dimethylbenz(a)anthracene (DMBA)-Induced Beast Cancer in the Rat, Cancer Lett, 2006.)
WORMWOOD VARIETY, ARTEMISIA ASINTHIUM: A NOVEL POTENTIAL COMPLEMENTARY AND ALTERNATIVE MEDICINE FOR BREAST CANCER?
Yes!
In Gowhar S et al.'s 2012 study, the researchers "investigated the in vitro anticancer activity
of crude extracts of the aerial parts of artemisia absinthium on estrogen-responsive (MCF-7) and estrogen-unresponsive human breast cancer (MDA-MB-231) cell lines."
The researchers stated that, "The apoptosis (cellular self-destruction) pathway was a novel target for cancer chemoprevention in recent studies of several chemopreventive agents."
Thus, in the same manner, can artemesia absinthium "modulate intracellular signaling mechanisms", to inhibit cell proliferation and promote apoptosis in these breast cancer cells? Apoptosis mechansims were upregulated: "Treatment with 25 μg/mL artemisia absinthium resulted in activation of caspase-7 (mitonchondrial pathway for apoptosis) and upregulation of Bad in MCF-7 cells, while exposure to 20 μg/mL artemisia absinthium induced upregulation of Bcl-2 protein in a time-dependent response in MDA-MB-231 cells."
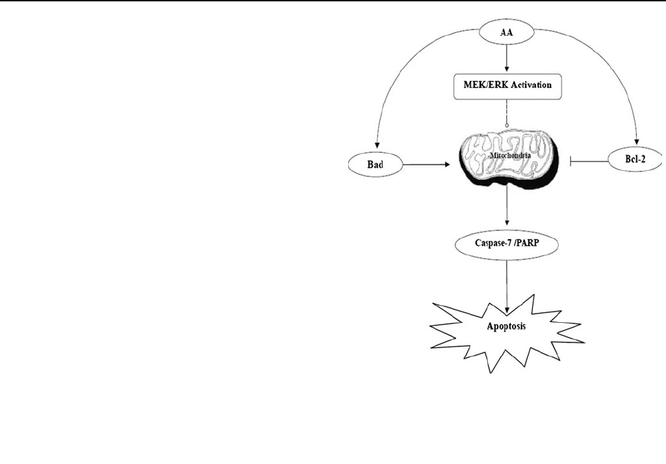
Conclusion: Artemisia absinthium was able to inhibit both estrogen-positive and estrogen-negative breast cancer cells via "the induction of apoptosis by regulating Bcl-2 family proteins and MEK/MAPK signaling."
"On the basis of the results of the current study, we propose that AA (artemisia absinthium) treatment triggers activation
of the MEK/ERK pathway (a chain of proteins relaying a signal from a receptor on the cell to the DNA in the nucleus of the cells), which then initiates the mitochondrial pathway of caspase activation, and regulates Bad and Bcl-2 family
proteins, culminating in the apoptotic death of MCF-7 and MDA-MB-231 cells (both hormone-positive and hormone-negative breast cancer cells)."
(See Gowhar S et al., Artemisia Absinithium (AA): A Novel Complementary and Alternative Medicine For Breast Cancer, Molecular Biology Reports, 2012.)
of the MEK/ERK pathway (a chain of proteins relaying a signal from a receptor on the cell to the DNA in the nucleus of the cells), which then initiates the mitochondrial pathway of caspase activation, and regulates Bad and Bcl-2 family
proteins, culminating in the apoptotic death of MCF-7 and MDA-MB-231 cells (both hormone-positive and hormone-negative breast cancer cells)."
(See Gowhar S et al., Artemisia Absinithium (AA): A Novel Complementary and Alternative Medicine For Breast Cancer, Molecular Biology Reports, 2012.)
THE HERB, BLACK WALNUT
BREAST CANCER STRATEGY - PLUMBAGIN (IN BLACK WALNUT) "EXHIBITS PROAPOPTOTIC, ANTIANGIOGENIC, AND ANTIMETASTATIC EFFECTS IN CANCER.". HOW ABOUT BREAST CANCER?
The 2016 Zhang XQ et al study found, after exposing breast cancer cells to different concentrations of plumbagin, that the "anti-proliferative effect of plumbagin is due to upregualtion of p53 (tumor suppressor gene) and p21 (regulates cell cycle progression), and suppression of G1 cell cycle regulators".
Conclusion: "Plumbagin exhibited significant anti-proliferative activity against human breast cancer cells!"
Zhang XQ et al., Plumbagin Shows Anti-Cancer Activity in Human Breast Cancer Cells by the Upregulation of p53 and p21 and Suppression of G1 Cell Cycle Regulators, Eur J Gynaecol Oncol, 2016.
The 2016 Zhang XQ et al study found, after exposing breast cancer cells to different concentrations of plumbagin, that the "anti-proliferative effect of plumbagin is due to upregualtion of p53 (tumor suppressor gene) and p21 (regulates cell cycle progression), and suppression of G1 cell cycle regulators".
Conclusion: "Plumbagin exhibited significant anti-proliferative activity against human breast cancer cells!"
Zhang XQ et al., Plumbagin Shows Anti-Cancer Activity in Human Breast Cancer Cells by the Upregulation of p53 and p21 and Suppression of G1 Cell Cycle Regulators, Eur J Gynaecol Oncol, 2016.
BREAST CANCER STRATEGY TO HELP PREVENT
BONE BREAK DOWN AND KILL CANCER CELLS (ESPECIALLY TRIPLE NEGATIVE)!
"We confirmed that plumbagin inhibited cell growth and enhanced apoptosis in human breast cancer cells, as well as inhibited the bone resorption induced by the tumor cells. Our data provide a solid basis for the future therapeutic application of plumbagin in the treatment of breast cancer bone metastases."
Sung B et al., 2011 READ THIS SECTION FOR FURTHER INFO
BONE BREAK DOWN AND KILL CANCER CELLS (ESPECIALLY TRIPLE NEGATIVE)!
"We confirmed that plumbagin inhibited cell growth and enhanced apoptosis in human breast cancer cells, as well as inhibited the bone resorption induced by the tumor cells. Our data provide a solid basis for the future therapeutic application of plumbagin in the treatment of breast cancer bone metastases."
Sung B et al., 2011 READ THIS SECTION FOR FURTHER INFO
BACKGROUND
"Juglans nigra, the eastern black walnut, a species of flowering tree in the walnut family, Juglandaceae, is native to eastern North American. It grows mostly in riparian zones, from southern Ontario, west to southeast South Dakota, south to Georgia, northern Florida and southwest to central Texas. Wild trees in the upper Ottawa Valley may be an isolated native population or may have derived from planted trees."
Some of the ingredients? "Black walnut drupes (having a pulpy middle, outer skin, and a hard and woody inner shell) usually contain juglone (5-hydroxyl-1.4-napthoquinone), tannins, and plumbagin (yellow quinone pigments)." (See http://en.wikipedia.org/wiki/Juglans_nigra#Alternative_medicine)
BLACK WALNUT AND PATHOGENS
"The Indians of America used the hulls of the American black walnut (juglans nigra) with its anti-parasitical, anti-bacterial and anti-viral properties to rid themselves of parasites."
(See http://www.drclark.net/en/about-dr-hulda-clark/discoveries-inventions-and-the-cause.)
ONE EXAMPLE: PLUMBAGIN IN BLACK WALNUT AND ITS EFFECT ON FASCIOLA GIGANTICA
The parasite, Fasiola gigantica, is a flatworm of the Trematoda class.
In Lorsuwannarat N et al's 2014 study, the researchers studied the effects of using plumbagin versus the drug, triclabendazole, on newly excysted juveniles and four week old immature parasites of Fasciola gigantica.
Results? For newly excysted juveniles, the decreased relative motility values were first observed at 1h incubation with 1μg/ml PB, and 90% of flukes were killed at 24h. In contrast, in triclabendazole-treated groups a 10-fold higher concentration of the drug (10μg/ml) resulted in only 9% dead parasites after 24h incubation. In 4-weeks-old juvenile parasites, plumbagin reduced the motility value at 10μg/ml with 100% of flukes dead after 3h, while the drug decreased motility values at the concentration of 100μg/ml but with only 5% of flukes killed at 24h"
In conclusion, "These data indicate that plumbagin had a greater fasciolicidal effect against immature stages of F. gigantica parasites than TCZ (the drug, triclabendazole), and warrant further studies for use as a potential new anthelmintic against Fasciola infections." (See Lorsuwannarat N et al., The In Vitro Anthelmintic Effects of Plumbagin on Newly Excysted and 4 Weeks-Old Juvenile Parasites of Fasciola Gigantica, Exp Parasitol, 2014.)
Why is this example of plumbagin and black walnut important? "Fascioliasis, an infection due to the food- and water-borne trematodes Fasciola hepatica and Fasciola gigantica, is among the most neglected of the neglected tropical diseases. Among the estimated 91.1 million humans at risk for infection worldwide, as many as 17 million may be infected. Certain areas of the world bear the burden of the highest prevalence of infection. There, school-age children are the most likely to be infected. In the United States, rare cases have been reported among immigrants from endemic areas, returned travelers to endemic regions, and individuals residing in Hawaii, California, and Florida. Indigenous cases have almost always been associated with consumption of watercress."
(See Robert Tolan Jr, MD., Fascioliasis Due to Fasciola Hepatica and Fasciola Gigantica Infection: An Update on This "Neglected" Neglected Tropical Disease, American Society for Clinical Pathology, 2011.)
PLUMBAGIN IN BLACK WALNUT AND BREAST CANCER CELLS
"Plumbagin has potent anti-proliferative and apoptotic activities in various types of human cancers, but the mechanisms underlying the anticancer activity are only partially understood. This compound dysregulates multiple pathways that play a crucial role in cancer cell proliferation, survival, invasion and metastasis "
In the 2012 Ju-Hee L et al. study, the researchers observed that past "results indicated that ROS (reactive oxygen species) are critical mediators of plumbagin cytotoxicity on human cancer".
But, how?
The researchers investigated phosphatidylinositol lipids. These phosphatidylinositol lipids" have been implicated in various cellular events such as cell survival, mitogenesis, and morphological changes. A number of phosphatidylinositol kinases (PIKs) are responsible for the activation of these lipids through the phosphorylation of the inositol ring."
The researchers observed that, " ...Plumbagin decreases the level of PI5K-1B, thereby leading to ROS generation for cytotoxicity in human breast cancer cells. ..... Until now, there has been no report about regulation of PI5K by plumbagin. Our report is the first to demonstrate that PI5K controls ROS generation as a molecular target of plumbagin. These results strongly suggest that targeted inhibition of PI5K by plumbagin plays a major role in ROS generation related to cytotoxicity."
Thus, the researchers found a PIK - "PI5K its 3 as a new molecular target of plumbagin for ROS generation."
(See Ju-Hee L et al., The Natural Anticancer Agent Plumbagin Induces Potent Cytotoxicity
in MCF-7 Human Breast Cancer Cells by Inhibiting a PI-5 Kinase for ROS Generation, PLOS One, 2012.)
PLUMBAGIN IN BLACK WALNUT AND BREAST CANCER THAT HAS SPREAD TO THE BONES IN MICE
80% of breast cancer patients with stage 4 breast cancer have cancer that has spread to the bones and created bone metastasis. Breast cancer that has spread to the bones "includes hypercalcemia of malignancy, severe bone pain, and debilitating skeletal morbidity.: And breast cancer has been associated "with osteolytic or mixed metastases."
What can be done? Bisphosonates are used for cancer that has spread to the bones, but there have been reports of bisphosonates increasing the risk of osteonecrosis of the jaw. Other things used are calcitonin, raloxifene, and teriparatide.
How about a safe strategy "to combat lytic and mixed bone lesions"?
Plumbagin!
In the 2011 Sung B et al. study, the researchers reported for the first time "that plumbagin can abrogate RANKL signaling". The significance of impeding RANKL signaling is that NF-kB is not activated, suppressing its participation in osteoclastogenesis.(bone break down).
"When examined for its ability to prevent human breast cancer-induced bone loss in animals, plumbagin (2 mg/kg body weight) administered via the intraperitoneal route significantly decreased osteolytic lesions, resulting in preservation of bone volume in nude mice bearing human breast tumors. Overall, our results indicate that plumbagin, a vitamin K analogue, is a potent inhibitor of osteoclastogenesis induced by tumor cells and of breast cancer-induced osteolytic metastasis through suppression of RANKL
signaling."
(See Sung B et al., Plumbagin Inhibits Osteoclastogenesis and Reduces Human Breast Cancer-Induced Osteolytic Bone Metastasis in Mice Through Suppression of RANKL Signaling, Mol Cancer Ther, 2011.)
PLUMBAGIN IN BLACK WALNUT AND BONE METASTASIS IN ESTROGEN-NEGATIVE BREAST CANCER CELLS AND IN MICE
In another study, this one a Wei Y et al. 2014 study, the researchers conducted experiments with plumbagin on a triple-negative breast cancer model that has the capability of spreading to the bone, both in an in vitro cell study and in mice.
The researchers found that, " ...Plumbagin effectively inhibited tumor cell growth in vitro concomitant with the induction of cell apoptosis; furthermore, plumbagin inhibited tumor cell growth in nude mice and suppressed the osteolysis induced by the MDA-MB-231SArfp (triple-negative) breast cancer cells."
Specifically, "Plumbagin (2.5–20 μmol/L) concentration-dependently inhibited the cell viability and induced apoptosis" in the in vitro breast cancer cells. After giving plumbagin to breast cancer-bearing mice, there was a 2-3 week delay in tumor growth, and the volume of the tumors was reduced by 44% -74%. In addition, imagine studies proved that plumbagin "reduced erosion area and prevented a decrease in bone tissue volume."
Conclusion: "We confirmed that plumbagin inhibited cell growth and enhanced apoptosis in human breast cancer cells, as well as inhibited the bone resorption induced by the tumor cells. Our data provide a solid basis for the future therapeutic application of plumbagin in the treatment of breast cancer bone metastases."
Good news for breast cancer patients, especially for those with triple-negative breast cancer
Wei Y et al., Plumbagin Attenuates Cancer Cell Growth and Osteoclast Formation in the Bone Microenvironment of Mice, Acta Pharmacologica Sinica, 2014.)
2015 Study - JUGLONE IN BLACK WALNUT AND ASCORBATE (VITAMIN C) IN BREAST CANCER CELLS AND IN EHRLICH ASCITES TUMOR IN MICE - DOES THE COMBO OF JUGLONE AND ASCORBATE HAVE A STRONGER EFFECT?
Yes!
It is known that high doses of vitamin C have an anti-cancer effect for their ability to deliver hydrogen peroxide (H2O2) to tumors.
What about combining vitamin C with juglone, which is found in black walnut?
Ourique et al., in their 2015 study, commented, "The activity of formulations including quinoid (juglone compounds) and ascorbate has been traditionally attributed to the enhanced generation of cellular ROS (reactive oxygen species) to levels that are above the protection capacity of cancer cells. The current study enhances the understanding of the antitumor mechanism of 1,4-naphthoquinones and ascorbate. The data highlight the effects of these molecules on the DNA and shows that when juglone or Q7 (a synthetically-derived juglone ) are administered together with ascorbate, a very damaging formulation is directed against the DNA of cancer cells in vitro and in vivo. The DNA of cancer cells thus degrades due to an oxidative stress caused by molecules that bind and intercalate into its strands. As a result, cell proliferation and tumor growth are inhibited, as shown in the following in vitro and in vivo."
Results in breast cancer cells: "The inhibition of proliferation was increased up to 3-fold when the naphthoquinones (juglones) were administered in combination with ascorbate." Why? "The PI3K/Akt pathway regulates several biological processes, including cell survival, proliferation, and differentiation. Upregulation of this pathway is observed in several types of cancer, and it can be associated with uncontrolled cell proliferation. As demonstrated, significant inhibition of the pAkt occurred in MCF-7 cells following treatment, most notably with juglone or Q7 in the presence of ascorbate."
Results in Ehrlich ascites carcinoma-bearing mice: There was some inhibition in the mice treated with juglone, Q7 or Q9, but up to a 60% inhibition of tumor growth with the addition of vitamin C. The chemo drug, doxorubicin, had a 90% inhibition rate. The researchers suggested that relative to tumor growth and survival, the potentiating effect of the treatment with ascorbate "was reproduced in vivo with statistical difference only in the case of juglone and Q7."
Conclusion: "Overall, it is possible to conclude that primarily juglone and Q7 combined with ascorbate have significant antitumor effects against MCF-7 cells in vitro and Ehrlich-ascites carcinoma in mice. The effects are the result of intercalation and oxidative attack on DNA of tumor cells and inhibition of the Akt pathway."
(See Ourique F et al., DNA Damage and Inhibition of Akt Pathway in MCF-7 Cells and Ehrlich Tumor in Mice Treated with 1,4-Naphthoquinones in Combination with Ascorbate, Oxid Med Cell Longev, 2015.)
"Juglans nigra, the eastern black walnut, a species of flowering tree in the walnut family, Juglandaceae, is native to eastern North American. It grows mostly in riparian zones, from southern Ontario, west to southeast South Dakota, south to Georgia, northern Florida and southwest to central Texas. Wild trees in the upper Ottawa Valley may be an isolated native population or may have derived from planted trees."
Some of the ingredients? "Black walnut drupes (having a pulpy middle, outer skin, and a hard and woody inner shell) usually contain juglone (5-hydroxyl-1.4-napthoquinone), tannins, and plumbagin (yellow quinone pigments)." (See http://en.wikipedia.org/wiki/Juglans_nigra#Alternative_medicine)
BLACK WALNUT AND PATHOGENS
"The Indians of America used the hulls of the American black walnut (juglans nigra) with its anti-parasitical, anti-bacterial and anti-viral properties to rid themselves of parasites."
(See http://www.drclark.net/en/about-dr-hulda-clark/discoveries-inventions-and-the-cause.)
ONE EXAMPLE: PLUMBAGIN IN BLACK WALNUT AND ITS EFFECT ON FASCIOLA GIGANTICA
The parasite, Fasiola gigantica, is a flatworm of the Trematoda class.
In Lorsuwannarat N et al's 2014 study, the researchers studied the effects of using plumbagin versus the drug, triclabendazole, on newly excysted juveniles and four week old immature parasites of Fasciola gigantica.
Results? For newly excysted juveniles, the decreased relative motility values were first observed at 1h incubation with 1μg/ml PB, and 90% of flukes were killed at 24h. In contrast, in triclabendazole-treated groups a 10-fold higher concentration of the drug (10μg/ml) resulted in only 9% dead parasites after 24h incubation. In 4-weeks-old juvenile parasites, plumbagin reduced the motility value at 10μg/ml with 100% of flukes dead after 3h, while the drug decreased motility values at the concentration of 100μg/ml but with only 5% of flukes killed at 24h"
In conclusion, "These data indicate that plumbagin had a greater fasciolicidal effect against immature stages of F. gigantica parasites than TCZ (the drug, triclabendazole), and warrant further studies for use as a potential new anthelmintic against Fasciola infections." (See Lorsuwannarat N et al., The In Vitro Anthelmintic Effects of Plumbagin on Newly Excysted and 4 Weeks-Old Juvenile Parasites of Fasciola Gigantica, Exp Parasitol, 2014.)
Why is this example of plumbagin and black walnut important? "Fascioliasis, an infection due to the food- and water-borne trematodes Fasciola hepatica and Fasciola gigantica, is among the most neglected of the neglected tropical diseases. Among the estimated 91.1 million humans at risk for infection worldwide, as many as 17 million may be infected. Certain areas of the world bear the burden of the highest prevalence of infection. There, school-age children are the most likely to be infected. In the United States, rare cases have been reported among immigrants from endemic areas, returned travelers to endemic regions, and individuals residing in Hawaii, California, and Florida. Indigenous cases have almost always been associated with consumption of watercress."
(See Robert Tolan Jr, MD., Fascioliasis Due to Fasciola Hepatica and Fasciola Gigantica Infection: An Update on This "Neglected" Neglected Tropical Disease, American Society for Clinical Pathology, 2011.)
PLUMBAGIN IN BLACK WALNUT AND BREAST CANCER CELLS
"Plumbagin has potent anti-proliferative and apoptotic activities in various types of human cancers, but the mechanisms underlying the anticancer activity are only partially understood. This compound dysregulates multiple pathways that play a crucial role in cancer cell proliferation, survival, invasion and metastasis "
In the 2012 Ju-Hee L et al. study, the researchers observed that past "results indicated that ROS (reactive oxygen species) are critical mediators of plumbagin cytotoxicity on human cancer".
But, how?
The researchers investigated phosphatidylinositol lipids. These phosphatidylinositol lipids" have been implicated in various cellular events such as cell survival, mitogenesis, and morphological changes. A number of phosphatidylinositol kinases (PIKs) are responsible for the activation of these lipids through the phosphorylation of the inositol ring."
The researchers observed that, " ...Plumbagin decreases the level of PI5K-1B, thereby leading to ROS generation for cytotoxicity in human breast cancer cells. ..... Until now, there has been no report about regulation of PI5K by plumbagin. Our report is the first to demonstrate that PI5K controls ROS generation as a molecular target of plumbagin. These results strongly suggest that targeted inhibition of PI5K by plumbagin plays a major role in ROS generation related to cytotoxicity."
Thus, the researchers found a PIK - "PI5K its 3 as a new molecular target of plumbagin for ROS generation."
(See Ju-Hee L et al., The Natural Anticancer Agent Plumbagin Induces Potent Cytotoxicity
in MCF-7 Human Breast Cancer Cells by Inhibiting a PI-5 Kinase for ROS Generation, PLOS One, 2012.)
PLUMBAGIN IN BLACK WALNUT AND BREAST CANCER THAT HAS SPREAD TO THE BONES IN MICE
80% of breast cancer patients with stage 4 breast cancer have cancer that has spread to the bones and created bone metastasis. Breast cancer that has spread to the bones "includes hypercalcemia of malignancy, severe bone pain, and debilitating skeletal morbidity.: And breast cancer has been associated "with osteolytic or mixed metastases."
What can be done? Bisphosonates are used for cancer that has spread to the bones, but there have been reports of bisphosonates increasing the risk of osteonecrosis of the jaw. Other things used are calcitonin, raloxifene, and teriparatide.
How about a safe strategy "to combat lytic and mixed bone lesions"?
Plumbagin!
In the 2011 Sung B et al. study, the researchers reported for the first time "that plumbagin can abrogate RANKL signaling". The significance of impeding RANKL signaling is that NF-kB is not activated, suppressing its participation in osteoclastogenesis.(bone break down).
"When examined for its ability to prevent human breast cancer-induced bone loss in animals, plumbagin (2 mg/kg body weight) administered via the intraperitoneal route significantly decreased osteolytic lesions, resulting in preservation of bone volume in nude mice bearing human breast tumors. Overall, our results indicate that plumbagin, a vitamin K analogue, is a potent inhibitor of osteoclastogenesis induced by tumor cells and of breast cancer-induced osteolytic metastasis through suppression of RANKL
signaling."
(See Sung B et al., Plumbagin Inhibits Osteoclastogenesis and Reduces Human Breast Cancer-Induced Osteolytic Bone Metastasis in Mice Through Suppression of RANKL Signaling, Mol Cancer Ther, 2011.)
PLUMBAGIN IN BLACK WALNUT AND BONE METASTASIS IN ESTROGEN-NEGATIVE BREAST CANCER CELLS AND IN MICE
In another study, this one a Wei Y et al. 2014 study, the researchers conducted experiments with plumbagin on a triple-negative breast cancer model that has the capability of spreading to the bone, both in an in vitro cell study and in mice.
The researchers found that, " ...Plumbagin effectively inhibited tumor cell growth in vitro concomitant with the induction of cell apoptosis; furthermore, plumbagin inhibited tumor cell growth in nude mice and suppressed the osteolysis induced by the MDA-MB-231SArfp (triple-negative) breast cancer cells."
Specifically, "Plumbagin (2.5–20 μmol/L) concentration-dependently inhibited the cell viability and induced apoptosis" in the in vitro breast cancer cells. After giving plumbagin to breast cancer-bearing mice, there was a 2-3 week delay in tumor growth, and the volume of the tumors was reduced by 44% -74%. In addition, imagine studies proved that plumbagin "reduced erosion area and prevented a decrease in bone tissue volume."
Conclusion: "We confirmed that plumbagin inhibited cell growth and enhanced apoptosis in human breast cancer cells, as well as inhibited the bone resorption induced by the tumor cells. Our data provide a solid basis for the future therapeutic application of plumbagin in the treatment of breast cancer bone metastases."
Good news for breast cancer patients, especially for those with triple-negative breast cancer
Wei Y et al., Plumbagin Attenuates Cancer Cell Growth and Osteoclast Formation in the Bone Microenvironment of Mice, Acta Pharmacologica Sinica, 2014.)
2015 Study - JUGLONE IN BLACK WALNUT AND ASCORBATE (VITAMIN C) IN BREAST CANCER CELLS AND IN EHRLICH ASCITES TUMOR IN MICE - DOES THE COMBO OF JUGLONE AND ASCORBATE HAVE A STRONGER EFFECT?
Yes!
It is known that high doses of vitamin C have an anti-cancer effect for their ability to deliver hydrogen peroxide (H2O2) to tumors.
What about combining vitamin C with juglone, which is found in black walnut?
Ourique et al., in their 2015 study, commented, "The activity of formulations including quinoid (juglone compounds) and ascorbate has been traditionally attributed to the enhanced generation of cellular ROS (reactive oxygen species) to levels that are above the protection capacity of cancer cells. The current study enhances the understanding of the antitumor mechanism of 1,4-naphthoquinones and ascorbate. The data highlight the effects of these molecules on the DNA and shows that when juglone or Q7 (a synthetically-derived juglone ) are administered together with ascorbate, a very damaging formulation is directed against the DNA of cancer cells in vitro and in vivo. The DNA of cancer cells thus degrades due to an oxidative stress caused by molecules that bind and intercalate into its strands. As a result, cell proliferation and tumor growth are inhibited, as shown in the following in vitro and in vivo."
Results in breast cancer cells: "The inhibition of proliferation was increased up to 3-fold when the naphthoquinones (juglones) were administered in combination with ascorbate." Why? "The PI3K/Akt pathway regulates several biological processes, including cell survival, proliferation, and differentiation. Upregulation of this pathway is observed in several types of cancer, and it can be associated with uncontrolled cell proliferation. As demonstrated, significant inhibition of the pAkt occurred in MCF-7 cells following treatment, most notably with juglone or Q7 in the presence of ascorbate."
Results in Ehrlich ascites carcinoma-bearing mice: There was some inhibition in the mice treated with juglone, Q7 or Q9, but up to a 60% inhibition of tumor growth with the addition of vitamin C. The chemo drug, doxorubicin, had a 90% inhibition rate. The researchers suggested that relative to tumor growth and survival, the potentiating effect of the treatment with ascorbate "was reproduced in vivo with statistical difference only in the case of juglone and Q7."
Conclusion: "Overall, it is possible to conclude that primarily juglone and Q7 combined with ascorbate have significant antitumor effects against MCF-7 cells in vitro and Ehrlich-ascites carcinoma in mice. The effects are the result of intercalation and oxidative attack on DNA of tumor cells and inhibition of the Akt pathway."
(See Ourique F et al., DNA Damage and Inhibition of Akt Pathway in MCF-7 Cells and Ehrlich Tumor in Mice Treated with 1,4-Naphthoquinones in Combination with Ascorbate, Oxid Med Cell Longev, 2015.)
DIGESTIVE ENZYMES
WHAT ARE DIGESTIVE ENZYMES?
"Molecules that catalyze the breakdown of large molecules (usually food) into smaller molecules." (Seehttp://medical-dictionary.thefreedictionary.com/digestive+enzymes.)
INGREDIENTS IN A TYPICAL SUPPLEMENT OF DIGESTIVE ENZYMES
Pepsin
Pancreatin
Ginger root
Lipase
Trypsin
Papain
Bromelain
PINEAPPLE! ONE DIGESTIVE ENZYME IS BROMELAIN. BROMELAIN COMES FROM PINEAPPLE
WHAT ARE DIGESTIVE ENZYMES?
"Molecules that catalyze the breakdown of large molecules (usually food) into smaller molecules." (Seehttp://medical-dictionary.thefreedictionary.com/digestive+enzymes.)
INGREDIENTS IN A TYPICAL SUPPLEMENT OF DIGESTIVE ENZYMES
Pepsin
Pancreatin
Ginger root
Lipase
Trypsin
Papain
Bromelain
PINEAPPLE! ONE DIGESTIVE ENZYME IS BROMELAIN. BROMELAIN COMES FROM PINEAPPLE
"Bromelain is a proteolytic enzyme, which can be helpful in treating cancer, because it helps restore balance to your immune system, among other cancer-fighting benefits "
Dr. Joseph Mercola
(http://articles.mercola.com/sites/articles/archive/2012/07/11/bromelain-enzyme-aid-cancer-treatment.aspx.)
EXPLORING BROMELAIN - ACTIVITY OF STEM PINEAPPLE'S BROMELAIN AND TUMORS
"Stem bromelain is a major cysteine proteinase, isolated from pineapple (Ananas comosus) stem. Its main medicinal use is recognized as digestive, in vaccine formulation, antitumoral and skin debrider for the treatment of burns."
Except for melanoma cases, "... All other tumor-bearing animals had a significantly increased survival index after bromelain treatment." After receiving 12.5 mg/kg of bromelain, the largest increase in survival was in mice with Ehrlich ascites carcinoma. In fact, "This antitumoral effect was superior to that of 5-5U, (a chemo drug) whose survival index was 263% relative to the untreated control."
"The antitumoral activity of bromelain against sarcoma and Ehrlich ascites, which are tumor models sensitive to immune system mediators, and the unchanged tumor progression in the metastatic model suggests that the antimetastatic action results from a mechanism independent of the primary antitumoral effect."
(See Baez R et al., In Vivo Antitumoral Activity of Stem Pineapple (Ananas comosus) Bromelain, Planta Med, 2007.)
ORAL BROMELAIN AND BREAST CANCER PATIENTS - BROMELAIN IMPROVES MONOCYTES AND ABILITY TO EAT DEBRIS
Macrophages are a type of white blood cells. Macrophages are derived from monocytes that travel around to infected areas and enlarge into macrophages that have the capability eat up debris, which is called phagocytosis. Macrophages can "engulf and digest cellular debris, foreign substances, microbes, cancer cells, and anything else that does not have the type of proteins specific to the surface of healthy body cells on its surface...." (See wikipedia.org.) This study examined the activity of monocytes in breast cancer patients.
In the Eckert K et al. 1999 study, breast cancer patients expressed lower macrophage and natural killer cell activities than healthy people.
The breast cancer patients were orally given bromelain. "Orally applied bromelain increased the reduced bMAK- and MAK-cell activity of patients monocytes about 2-fold. When the patients were classified on the basis of bromelain effects on the monocytic cytotoxicity into bromelain responders and nonresponders, about 40% of the patients responded to bromelain with an increase of cytotoxicity from 7.8% to 54% (bMAK-cell activity) and from 16% to 47% (MAK-cell activity)."
Conclusion: "These data suggest, that orally applied bromelain stimulates the deficient monocytic cytotoxicity of mammary tumor patients, which may partially explain its proposed antitumor activity."
EDITORS' NOTE:: Although it not known how, precisely, bromelain was able to increase the cytotoxicity of the monocytes, it is significant information that breast cancer patients can boost their immune systems. Monocytes, as written supra are not only the biggest type of white blood cell in the immune system, but they have the capability of fending off viruses, bacteria, and fungi.
(See Eckert K et al., Effects of Oral Bromelain Administration on the Impaired Immunocytotoxicity of Mononuclear Cells from Mammary Tumor Patients, Oncol Rep, 1999.)
Bromelain Induces Autophagy, Apoptosis in Breast Cancer Cells
Autophagy is the self-eating of damaged cells in the body. "It maintains homeostasis or normal functioning by protein degradation and turnover of the destroyed cell organelles for new cell formation. ... Autophagy also kills the cells under certain conditions. These are forms of programmed cell death and are called autophagic cell death. Programmed cell death is commonly termed apoptosis." (See http://www.news-medical.net/health/What-is-Autophagy.aspx.)
In Bhul K et al's 2010 study, estrogen-positive breast cancer cells exposed to bromelain showed delayed growth inhibitory response and induction of autophagy, identified by monodansylcadaverine (marker of autophagy) localization. It was succeeded by apoptotic cell death, evident by sub-G1 cell fraction and apoptotic features like chromatin condensation and nuclear cleavage."
Conclusion: "Autophagy-inducing property of bromelain can be further exploited in breast cancer therapy."
(See Bhul K et al., Pineapple Bromelain Induces Autophagy, Facilitating Apoptotic Response in Mammary Carcinoma Cells, Biofactors, 2010.)
Dr. Joseph Mercola
(http://articles.mercola.com/sites/articles/archive/2012/07/11/bromelain-enzyme-aid-cancer-treatment.aspx.)
EXPLORING BROMELAIN - ACTIVITY OF STEM PINEAPPLE'S BROMELAIN AND TUMORS
"Stem bromelain is a major cysteine proteinase, isolated from pineapple (Ananas comosus) stem. Its main medicinal use is recognized as digestive, in vaccine formulation, antitumoral and skin debrider for the treatment of burns."
Except for melanoma cases, "... All other tumor-bearing animals had a significantly increased survival index after bromelain treatment." After receiving 12.5 mg/kg of bromelain, the largest increase in survival was in mice with Ehrlich ascites carcinoma. In fact, "This antitumoral effect was superior to that of 5-5U, (a chemo drug) whose survival index was 263% relative to the untreated control."
"The antitumoral activity of bromelain against sarcoma and Ehrlich ascites, which are tumor models sensitive to immune system mediators, and the unchanged tumor progression in the metastatic model suggests that the antimetastatic action results from a mechanism independent of the primary antitumoral effect."
(See Baez R et al., In Vivo Antitumoral Activity of Stem Pineapple (Ananas comosus) Bromelain, Planta Med, 2007.)
ORAL BROMELAIN AND BREAST CANCER PATIENTS - BROMELAIN IMPROVES MONOCYTES AND ABILITY TO EAT DEBRIS
Macrophages are a type of white blood cells. Macrophages are derived from monocytes that travel around to infected areas and enlarge into macrophages that have the capability eat up debris, which is called phagocytosis. Macrophages can "engulf and digest cellular debris, foreign substances, microbes, cancer cells, and anything else that does not have the type of proteins specific to the surface of healthy body cells on its surface...." (See wikipedia.org.) This study examined the activity of monocytes in breast cancer patients.
In the Eckert K et al. 1999 study, breast cancer patients expressed lower macrophage and natural killer cell activities than healthy people.
The breast cancer patients were orally given bromelain. "Orally applied bromelain increased the reduced bMAK- and MAK-cell activity of patients monocytes about 2-fold. When the patients were classified on the basis of bromelain effects on the monocytic cytotoxicity into bromelain responders and nonresponders, about 40% of the patients responded to bromelain with an increase of cytotoxicity from 7.8% to 54% (bMAK-cell activity) and from 16% to 47% (MAK-cell activity)."
Conclusion: "These data suggest, that orally applied bromelain stimulates the deficient monocytic cytotoxicity of mammary tumor patients, which may partially explain its proposed antitumor activity."
EDITORS' NOTE:: Although it not known how, precisely, bromelain was able to increase the cytotoxicity of the monocytes, it is significant information that breast cancer patients can boost their immune systems. Monocytes, as written supra are not only the biggest type of white blood cell in the immune system, but they have the capability of fending off viruses, bacteria, and fungi.
(See Eckert K et al., Effects of Oral Bromelain Administration on the Impaired Immunocytotoxicity of Mononuclear Cells from Mammary Tumor Patients, Oncol Rep, 1999.)
Bromelain Induces Autophagy, Apoptosis in Breast Cancer Cells
Autophagy is the self-eating of damaged cells in the body. "It maintains homeostasis or normal functioning by protein degradation and turnover of the destroyed cell organelles for new cell formation. ... Autophagy also kills the cells under certain conditions. These are forms of programmed cell death and are called autophagic cell death. Programmed cell death is commonly termed apoptosis." (See http://www.news-medical.net/health/What-is-Autophagy.aspx.)
In Bhul K et al's 2010 study, estrogen-positive breast cancer cells exposed to bromelain showed delayed growth inhibitory response and induction of autophagy, identified by monodansylcadaverine (marker of autophagy) localization. It was succeeded by apoptotic cell death, evident by sub-G1 cell fraction and apoptotic features like chromatin condensation and nuclear cleavage."
Conclusion: "Autophagy-inducing property of bromelain can be further exploited in breast cancer therapy."
(See Bhul K et al., Pineapple Bromelain Induces Autophagy, Facilitating Apoptotic Response in Mammary Carcinoma Cells, Biofactors, 2010.)
DIGESTIVE ENZYMES AND CANCER
WHAT DIGESTIVE ENZYMES DO
"Degrade and chew up fibrin (cancer cells are coated with a protein fibrin coating), unmasking cell antigens, leaving them open for attack by immune fighters ...."
Dr. Anthony Cichoke, 2011 (For a wonderful discussion of enzymes, go to https://www.youtube.com/watch?v=hpJXyx22Jic.)
In 2000, Lipinksi B et al. presented a tumor coat theory. It is known that "tumor cells can escape detection and attack by the immune system in most cancer patients. The tumor dons a 'coat' of the host's own protein on its cell surface. The coat is composed of fibrin and of a polymeric form of human serum albumin (HSA) which, by contrast to pure fibrin, is resistant to fibrinolytic degradation. Such a coated tumor appears as 'self' to the immune system, and thus is not detected as a tumor by the immune system (i.e.. natural killer cells). When tumors are prepared for in vitro assays against drugs, they are routinely treated with proteolytic enzymes (e.g. pepsin, or chymotrypsin, etc.) which dissolve the protein coat, exposing the tumor cell surface to the drug. Thus, the in vivo existence of a coat on the tumor surface may explain why some drugs have little or no effect in vivo, while the same drugs are active in vitro."
(See Lipinski B et al.,Resistance of Cancer Cells to Immune Recognition and Killing, Med Hypotheses, 2000.)
WHAT DIGESTIVE ENZYMES DO
"Degrade and chew up fibrin (cancer cells are coated with a protein fibrin coating), unmasking cell antigens, leaving them open for attack by immune fighters ...."
Dr. Anthony Cichoke, 2011 (For a wonderful discussion of enzymes, go to https://www.youtube.com/watch?v=hpJXyx22Jic.)
In 2000, Lipinksi B et al. presented a tumor coat theory. It is known that "tumor cells can escape detection and attack by the immune system in most cancer patients. The tumor dons a 'coat' of the host's own protein on its cell surface. The coat is composed of fibrin and of a polymeric form of human serum albumin (HSA) which, by contrast to pure fibrin, is resistant to fibrinolytic degradation. Such a coated tumor appears as 'self' to the immune system, and thus is not detected as a tumor by the immune system (i.e.. natural killer cells). When tumors are prepared for in vitro assays against drugs, they are routinely treated with proteolytic enzymes (e.g. pepsin, or chymotrypsin, etc.) which dissolve the protein coat, exposing the tumor cell surface to the drug. Thus, the in vivo existence of a coat on the tumor surface may explain why some drugs have little or no effect in vivo, while the same drugs are active in vitro."
(See Lipinski B et al.,Resistance of Cancer Cells to Immune Recognition and Killing, Med Hypotheses, 2000.)
DIGESTIVE ENZYMES AND TUMORS - HOW EFFECTIVE ARE TRYPSIN, CHYMOTRYPSIN, AND PAPAIN AGAINST TUMORS?
In the Wald M et al. 2008 monograph, the digestive enzymes, trypsin, chymotrypsin, and papain demonstrated "a significant inhibition of growth of both the primary tumor and the metastatic disseminations."
Overall, "The survival in animals treated with proteases is significantly longer than in untreated animals."
Conclusion: "The results confirm the fundamental correlation between early initiation of therapy and consequent growth of the tumorous disease. Comparable results have been shown in solid tumors in animal models (melanoma and Lewis lung carcinoma) and in human tumors (pancreatic and breast cancers)."
(See Wald M et al., Exogenous Proteases Confer A Significant Chemopreventive Effect in Experimental Tumor Models, Integr Cancer Ther, 2008.)
TRYPSIN, CHYMOTRYPSIN, AND PAPAIN OR BROMELAIN - EVALUATION OF ENZYME THERAPY
In the Beuth J et al. 2008 study, " EBM level II clinical studies, which are accepted by the European Union to show safety and efficacy of medical treatments, were performed to evaluate the benefit of complementary systemic enzyme therapy in cancer patients suffering from breast and colorectal cancers and plasmacytoma."
Results: "These studies demonstrated that systemic enzyme therapy significantly decreased tumor-induced and therapy-induced side effects and complaints such as nausea, gastrointestinal complaints, fatigue, weight loss, and restlessness and obviously stabilized the quality of life."
(See Beuth J et al., Proteolytic Enzyme Therapy in Evidence-Based Complementary Oncology: Fact or Fiction?, Integr Cancer Ther, 2008.)
ORAL ENZYMES FOLLOWING BREAST CANCER SURGERY - DURING TREATMENT
In the Beuth J et al. study, the researchers gave oral enzymes to breast cancer patients to see if the enzymes would improve their quality of life during treatment.
Specifically, breast cancer patients who had completed their surgeries and who were undergoing either radiation, chemo, or hormone treatment were enrolled in the study. Those patients who were given the oral enzymes were followed for 485 days, while the breast cancer patients who did not have the oral enzymes were followed for 213 days.
Could the oral enzymes reduce " typical disease- or therapy-associated signs and symptoms (gastrointestinal symptoms, mental symptoms, dyspnoea, headache, tumour pain, cachexia, skin disorders, infections, and side effects associated with the antineoplastic therapy?"
Yes!
Results: For 75% of the patients on enzymes and 55% of the control group not on enzymes, the physician recorded "no signs and symptoms". .... "A clear reduction in the side effects of radiotherapy and chemotherapy was documented in 75% of the test group and 55% of the control group." In addition,"Analysis of survival, recurrence, and metastasis demonstrated a reduced number of events in the test group. There was evidence of a beneficial influence of oral enzymes on time to event, although the median observation time was too short in these breast cancer patients to draw definite conclusions."
Thus, not only is there an improvement in the quality of life but, when given oral enzymes, there is "evidence that the patients may also gain benefit by a prolongation of the time to event for cancer recurrence, metastasis, and survival."
(See Beuth J et al., Impact of Complementary Oral Enzyme Application on the Postoperative Treatment Results of Breast Cancer Patients - Results of an Epidemiological Multicentre Retrolective Cohort Study, Cancer Chemother Pharmacol, 2001.)
DR. NICHOLAS GONZALEZ AND PANCREATIC ENZYMES
In their 1999 study, Drs. Nicholas Gonzalez and Linda Isaacs used large doses of proteolytic enzymes in pancreatic cancer patients.
"Historically, large doses of proteolytic enzymes, along with diet, nutritional supplements, and 'detoxification' procedures, have been used in alternative therapies to treat all forms of cancer, without formal clinical studies to support their use. A 2-year, unblinded, 1-treatment arm, 10-patient, pilot prospective case study was used to assess survival in patients suffering inoperable stage II-IV pancreatic adenocarcinoma treated with large doses of orally ingested pancreatic enzymes, nutritional supplements, detoxification procedures, and an organic diet."
Results: At the end of the study, " Of 11 patients (one had dropped out and another entered the study), 9 (81%) survived one year, 5 (45%) survived two years, and at this time, 4 have survived three years. Two patients are alive and doing well: one at three years and the other at four years. These results are far above the 25% survival at one year and 10% survival at two years for all stages of pancreatic adenocarcinoma."
Conclusion: "This pilot study suggests that an aggressive nutritional therapy with large doses of pancreatic enzymes led to significantly increased survival over what would normally be expected for patients with inoperable pancreatic adenocarcinoma."
(See Gonzalez NJ and Isaacs LL, Evaluation of Pancreatic Proteolytic Enzyme Treatment of Adenomacarcinoma of the Pancreas, with Nutrition and Detoxification Support, Nutr Cancer, 1999. ..... Also, see www.dr-gonzalez.com to read about their enzyme protocol. Note that Drs. Gonzalez and Isaacs use a "Pancreas Product (For Cancer Patients): The main anti-cancer supplement is a specially manufactured pancreas product -containing naturally occurring enzymes - made from pig pancreas. ... Cancer patients on this regimen take up to 45 grams of pancreas product a day, taken orally and spread throughout the day.)
In the Wald M et al. 2008 monograph, the digestive enzymes, trypsin, chymotrypsin, and papain demonstrated "a significant inhibition of growth of both the primary tumor and the metastatic disseminations."
Overall, "The survival in animals treated with proteases is significantly longer than in untreated animals."
Conclusion: "The results confirm the fundamental correlation between early initiation of therapy and consequent growth of the tumorous disease. Comparable results have been shown in solid tumors in animal models (melanoma and Lewis lung carcinoma) and in human tumors (pancreatic and breast cancers)."
(See Wald M et al., Exogenous Proteases Confer A Significant Chemopreventive Effect in Experimental Tumor Models, Integr Cancer Ther, 2008.)
TRYPSIN, CHYMOTRYPSIN, AND PAPAIN OR BROMELAIN - EVALUATION OF ENZYME THERAPY
In the Beuth J et al. 2008 study, " EBM level II clinical studies, which are accepted by the European Union to show safety and efficacy of medical treatments, were performed to evaluate the benefit of complementary systemic enzyme therapy in cancer patients suffering from breast and colorectal cancers and plasmacytoma."
Results: "These studies demonstrated that systemic enzyme therapy significantly decreased tumor-induced and therapy-induced side effects and complaints such as nausea, gastrointestinal complaints, fatigue, weight loss, and restlessness and obviously stabilized the quality of life."
(See Beuth J et al., Proteolytic Enzyme Therapy in Evidence-Based Complementary Oncology: Fact or Fiction?, Integr Cancer Ther, 2008.)
ORAL ENZYMES FOLLOWING BREAST CANCER SURGERY - DURING TREATMENT
In the Beuth J et al. study, the researchers gave oral enzymes to breast cancer patients to see if the enzymes would improve their quality of life during treatment.
Specifically, breast cancer patients who had completed their surgeries and who were undergoing either radiation, chemo, or hormone treatment were enrolled in the study. Those patients who were given the oral enzymes were followed for 485 days, while the breast cancer patients who did not have the oral enzymes were followed for 213 days.
Could the oral enzymes reduce " typical disease- or therapy-associated signs and symptoms (gastrointestinal symptoms, mental symptoms, dyspnoea, headache, tumour pain, cachexia, skin disorders, infections, and side effects associated with the antineoplastic therapy?"
Yes!
Results: For 75% of the patients on enzymes and 55% of the control group not on enzymes, the physician recorded "no signs and symptoms". .... "A clear reduction in the side effects of radiotherapy and chemotherapy was documented in 75% of the test group and 55% of the control group." In addition,"Analysis of survival, recurrence, and metastasis demonstrated a reduced number of events in the test group. There was evidence of a beneficial influence of oral enzymes on time to event, although the median observation time was too short in these breast cancer patients to draw definite conclusions."
Thus, not only is there an improvement in the quality of life but, when given oral enzymes, there is "evidence that the patients may also gain benefit by a prolongation of the time to event for cancer recurrence, metastasis, and survival."
(See Beuth J et al., Impact of Complementary Oral Enzyme Application on the Postoperative Treatment Results of Breast Cancer Patients - Results of an Epidemiological Multicentre Retrolective Cohort Study, Cancer Chemother Pharmacol, 2001.)
DR. NICHOLAS GONZALEZ AND PANCREATIC ENZYMES
In their 1999 study, Drs. Nicholas Gonzalez and Linda Isaacs used large doses of proteolytic enzymes in pancreatic cancer patients.
"Historically, large doses of proteolytic enzymes, along with diet, nutritional supplements, and 'detoxification' procedures, have been used in alternative therapies to treat all forms of cancer, without formal clinical studies to support their use. A 2-year, unblinded, 1-treatment arm, 10-patient, pilot prospective case study was used to assess survival in patients suffering inoperable stage II-IV pancreatic adenocarcinoma treated with large doses of orally ingested pancreatic enzymes, nutritional supplements, detoxification procedures, and an organic diet."
Results: At the end of the study, " Of 11 patients (one had dropped out and another entered the study), 9 (81%) survived one year, 5 (45%) survived two years, and at this time, 4 have survived three years. Two patients are alive and doing well: one at three years and the other at four years. These results are far above the 25% survival at one year and 10% survival at two years for all stages of pancreatic adenocarcinoma."
Conclusion: "This pilot study suggests that an aggressive nutritional therapy with large doses of pancreatic enzymes led to significantly increased survival over what would normally be expected for patients with inoperable pancreatic adenocarcinoma."
(See Gonzalez NJ and Isaacs LL, Evaluation of Pancreatic Proteolytic Enzyme Treatment of Adenomacarcinoma of the Pancreas, with Nutrition and Detoxification Support, Nutr Cancer, 1999. ..... Also, see www.dr-gonzalez.com to read about their enzyme protocol. Note that Drs. Gonzalez and Isaacs use a "Pancreas Product (For Cancer Patients): The main anti-cancer supplement is a specially manufactured pancreas product -containing naturally occurring enzymes - made from pig pancreas. ... Cancer patients on this regimen take up to 45 grams of pancreas product a day, taken orally and spread throughout the day.)
If you would like to consider this herbal formula of cloves, wormwood, black walnut, and digestive enzymes, go to:
http://www.drclark.net/en/cleanses/beginners/herbal-parasite-cleanse
http://www.drclark.net/en/cleanses/beginners/herbal-parasite-cleanse